Chronic pain, or persistent pain that frequently interferes with life and professional activities, affects approximately one in five people in the United States.1 Chronic pain is one of the most common reasons individuals seek medical care. It is often a symptom of common chronic conditions including but not limited to arthritis, fibromyalgia, cancer, diabetes, and injury/trauma. People with chronic pain may experience reduced quality of life, poor mental health, and addiction.
The Pain Cycle
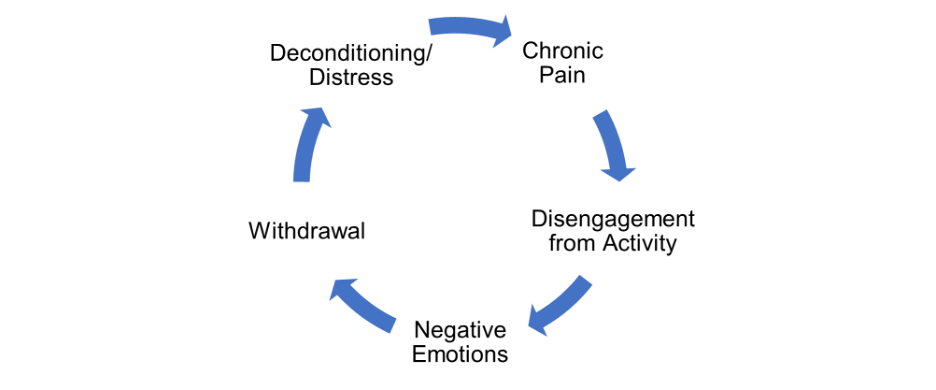
For many people, pain is increased and maintained by a “pain cycle” by which physical pain leads one to disengage from meaningful life activities (e.g., work, social obligations, physical activity). Disengaging leads to negative emotions or depression symptoms (e.g., sadness, hopelessness, isolation, anxiety). These psychological symptoms make it even more difficult to re-engage in life activities (including those important for pain management), causing one to withdraw, which can cause physical deconditioning (e.g., muscular atrophy) and distress and exacerbate and perpetuate the physical pain.2 This cycle of pain and low mood can go on for decades, leaving people feeling as though they’re “prisoners to pain.”
Substance Use and Addiction in Chronic Pain
Stuck in the pain cycle, people may look for escapes and ultimately find themselves misusing substances and even developing addiction. Pain management typically involves the use of potentially addictive prescription medications such as opioids.
In the past several years, light has been shed on the “opioid epidemic,” and the high rates of opioid misuse, dependency, and addiction. Unfortunately, people often feel desperate for a solution to chronic pain and depression and may come to rely on addictive medications to cope.3 In addition, people with chronic pain are susceptible to misuse other non-prescribed substances like alcohol to help “numb” the pain at the cost of their physical and mental health.4
Together these experiences lead to a cluster of symptoms of chronic pain, depression, and addiction, all of which can be incredibly isolating and debilitating.5 This combination of symptoms can have effects on not just the patient but also family members and friends who may need to serve as caregivers, may notice strain on their relationships, and may find that their lifestyles and social activities are disrupted.1
Psychological Treatments for Pain Management
Considering the potential risks for depression in those suffering with pain and their loved ones, some may look for non-pharmacological, psychological approaches to either supplement or replace their current pain management regiment. Fortunately, there are psychological or behavioral treatments that work as nice complements and alternatives to medication management of chronic pain.5 These treatments do NOT assume that the pain is “in your head,” nor do they attempt to take the pain away entirely. Behavioral treatments focus on equipping one to live full lives despite pain and maximize quality of life while coping with chronic pain.
Cognitive Behavioral Therapy
Perhaps the most well-evidenced non-medication approach to pain management is cognitive behavioral therapy for chronic pain (CBT-CP).1 CBT-CP helps individuals identify links between their thoughts, feelings, and behaviors to find targets for change and to break the pain cycle. It includes components intended to address concerns related to substance use, sleep/insomnia, and social/relationship problems.
Acceptance and Commitment Therapy
Another effective treatment for chronic pain is Acceptance and Commitment Therapy (ACT).6 ACT can help individuals accept some of the unpleasant feelings they have about their pain and its impact on their lives. It facilitates a sense of control over pain and its impact. It clarifies one’s most important values to help them live meaningful and purposeful lives in the face of pain. It also has shown to be effective in those dealing with substance use and addiction.7
Chronic pain and its consequences can have a tremendous impact on mental and physical health and quality of life of entire families; however, these treatments aimed to break the pain cycle and expand the lives of those coping with pain are effective. Non-pharmacological treatments for pain can be an opportunity to learn a range of coping skills and simultaneously address concerns related to pain, depression, and addiction, to ultimately improve and expand lives.
Everyone’s experience with pain, depression, and addiction is unique. At Fifth Avenue Psychiatry, treatment can be tailored to the individual to manage this set of symptoms in a discrete, confidential, and supportive setting. These psychological treatments for chronic pain can be applied to help enhance one’s functioning in their personal and professional lives.
Our team of Manhattan addiction professionals and psychiatrists provide discrete, personalized, and professional addiction and substance abuse therapy. Dr. Glazer has been recognized as a Castle Connolly Top Doctor since 2015.
References
- Kuehn, B. (2018). Chronic pain prevalence. Jama, 320(16), 1632-1632.
- Murphy, J. L., Cordova, M. J., & Dedert, E. A. (2022). Cognitive behavioral therapy for chronic pain in veterans: Evidence for clinical effectiveness in a model program. Psychological services, 19(1), 95.
- Vowles, K. E., McEntee, M. L., Julnes, P. S., Frohe, T., Ney, J. P., & Van Der Goes, D. N. (2015). Rates of opioid misuse, abuse, and addiction in chronic pain: a systematic review and data synthesis. Pain, 156(4), 569-576.
- Witkiewitz, K. & Vowles, K.E. (2018) Alcohol and opioid use, co-use, and chronic pain I the context of the opioid epidemic: A critical review. Alcoholism: clinical and experimental research, 42 (3), 478-488
- Majeed, M. H., & Sudak, D. M. (2017). Cognitive behavioral therapy for chronic pain—One therapeutic approach for the opioid epidemic. Journal of Psychiatric Practice®, 23(6), 409-414.
- Hughes, L. S., Clark, J., Colclough, J. A., Dale, E., & McMillan, D. (2017). Acceptance and commitment therapy (ACT) for chronic pain. The Clinical journal of pain, 33(6), 552-568.
Osaji, J., Ojimba, C., & Ahmed, S. (2020). The use of acceptance and commitment therapy in substance use disorders: a review of literature. Journal of clinical medicine research, 12(10), 629.